Minimally Invasive Bunion Surgery
Over the last century, more than 100 different procedures have been described for correcting bunions. The ultimate goal of any bunion surgery is to restore the normal shape and biomechanics of the foot in order to reduce pain and allow return to normal shoewear.
Minimally Invasive (Keyhole) Bunion Correction
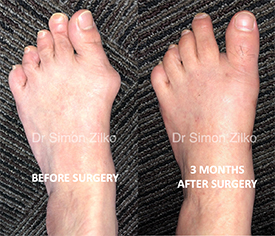
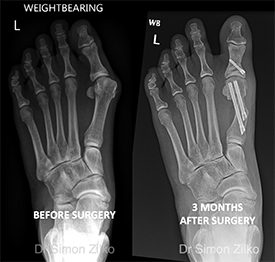
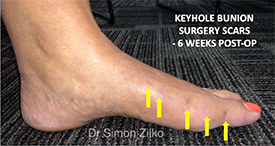
Procedure
Patients are admitted to hospital on the day of surgery, and the procedure is done under a general anaesthetic with an ankle anaesthetic block. The ankle block is the application of local anaesthetic around the ankle, which usually provides pain relief for up to 12 hours after the surgery.
In general, if a person has surgery on one foot then they can go home from hospital on the same day. If they have bunions corrected on both feet then usually an overnight stay is recommended.
Recovery & Rehabilitation
Patients are allowed to walk full weightbearing in a stiff-soled surgical shoe from the day of surgery. In general, crutches may be needed for the first 5-10 days after surgery for comfort and balance, but it is fine to discard the crutches earlier if able.
The local anaesthetic block usually makes the foot pain-free for 6-12 hours. Strong pain killers are usually only needed for the first 3-7 days, after which paracetamol is generally all that’s required.
After discharge, the dressings and bandages must all stay intact and dry until review 2 weeks after surgery. During this time, it is particularly important to elevate the foot for most of the day, with “toes above the nose”! Strict elevation helps swelling come down faster, which means less pain and less chance of wound healing issues.
At 2 weeks after surgery, the wounds are checked. Range of motion exercises and rehabilitation are started once the incisions have healed. A simple exercise of gently manually moving the great toe up and down is important to prevent stiffness.
After 2-3 weeks, patients can transition to wearing a supportive shoe as swelling and comfort allows. Any shoe must have a firm supportive sole, and should be straight over the inner aspect (so as not to push the big toe towards the little toes).
Return to Work & Activities
Driving: For left foot surgery, patients can drive an automatic car as soon as they’re walking well and off all strong painkillers (usually from 1 week). For right foot surgery or those with a manual car, patients can drive once they’re in a normal shoe, have minimal pain and can safely operate the brake/clutch (usually 3-6 weeks post-surgery).
Work: Office and desk-job workers can go back to work after 2-3 weeks, but those doing manual jobs on their feet often need a full 6 weeks off.
Exercise: Most patients can use an exercise bike or elliptical trainer after 4 weeks, and can swim after 4-6 weeks. Impact exercises such as running or jumping are usually possible after 3 months.
The bone cuts take around 12 weeks to fully heal, and most of the swelling diminishes by 3-4 months. By 6 months most patients have returned to their normal activities without pain or discomfort.
What should patients know before considering bunion surgery?
There’s no such thing as risk-free surgery, so patients need to be having enough problems with their feet to warrant surgical intervention, and of course be aware of the potential risks. Minimally invasive surgery is not indicated for some types of bunion, particularly when arthritis is present.
Recurrence of the bunion is possible, and depends on both the severity of the patient’s pre-operative deformity, the surgical technique employed, as well as their age. Infection rates are generally very low, as are the risks of nerve damage, stiffness, or problems with bone healing.
Conditions like diabetes, peripheral vascular disease or long-term use of immunosuppressant drugs (eg steroids) are possible contraindications to surgery, and patients with these conditions require careful evaluation by an orthopaedic surgeon (medical practitioner).
Bunion surgery is covered by both Medicare and private health funds only when performed by an orthopaedic surgeon (medical doctor).
Please note that podiatrists performing surgery are not medical doctors; have not undergone medical school and teaching hospital surgical training for 13-15 years like orthopaedic surgeons; are unable to prescribe all antibiotics, painkillers, anti-emetics and other medications that may be required after surgery; and are not covered at all by Medicare for surgery.
You will need the Adobe Reader to view and print these documents. ![]()
